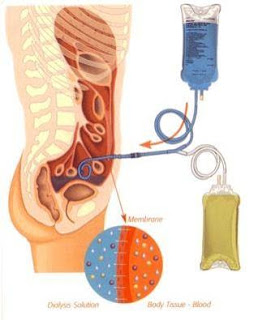
While it has long been postulated that ACE inhibition may help PD patients preserve their residual renal function, there may be another benefit to angiotensin blockade: preservation of peritoneal membrane transport . Last year, a group from the Netherlands analyzed a cohort of incident PD patients in the Netherlands Cooperative Study on Adequacy of Dialysis, and found that the D/P creatinine ratio in patients on ACE inhibitors increased at a significantly slower rate than those not on ACEIs. An increase in small solute transport is thought to represent an increase in membrane neoangiogenesis, likely mediated by TGF-beta and VEGF, which have also been shown to promote peritoneal fibrosis. The study’s authors postulate that ACE inhibitor-mediated downregulation of TGF beta and VEGF explains the slower rate of membrane transport alteration. While no difference in mortality or residual renal function was noted, there did appear to be a beneficial effect on technique survival, one which might have reached statistical significance if the study had continued beyond its 2-4 year duration. Ultrafiltration efficacy was not analyzed, but one might expect increased UF difficulty with increased membrane transport.
Patients on PD have a number of reasons to be on ACE inhibitors, including their high rates of cardiovascular disease and hypertension, as well as desire to preserve residual renal function. Membrane preservation may be yet another reason to add to the list.