Here’s a case I saw on the consult service last week which demonstrates the utility of examining the urine sediment yourself.
The clinical scenario: a 50 year-old male with a history of hepatitis C liver disease who was admitted with altered mental status and a rising bilirubin. About a week into his hospital stay, his creatinine began rising from its baseline of about 0.8 to as high as 3.5 mg/dL. His T-bili had made it up to 18 and he was being evaluated for a liver transplant. He had received some iv contrast a day before his creatinine started rising, and before we examined the urine sediment I was pretty certain the diagnosis was going to be either hepatorenal syndrome or contrast-induced nephropathy.
Interestingly, his urine showed the following (this is a photo of the actual sediment): WBC casts!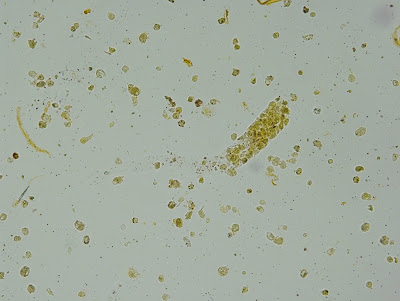 The WBC casts were not difficult to find and there were plenty of WBCs present in a non-Foleyed specimen. It turns out that the patient had had a single blood culture which was positive for MSSA and was being treated with iv nafcillin. The diagnosis here is acute interstitial nephritis (AIN), and we are recommending a short course of oral steroids (though I realize that this is certainly a controversial topic).
The WBC casts were not difficult to find and there were plenty of WBCs present in a non-Foleyed specimen. It turns out that the patient had had a single blood culture which was positive for MSSA and was being treated with iv nafcillin. The diagnosis here is acute interstitial nephritis (AIN), and we are recommending a short course of oral steroids (though I realize that this is certainly a controversial topic).
The hospital’s automated urinalysis–which over the course of this year I have learned to not put much faith in outside of the dipstick analysis–did not make note of any casts, and is a clear example that a nephrologist’s evaluation of the urine sediment still is an essential part of the consult evaluation.

