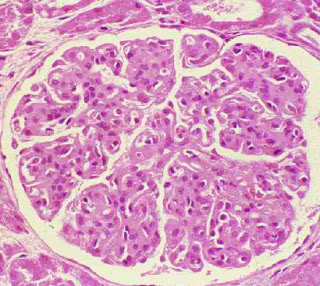
 Cryoglobulinemia is characterized by the presence of circulating antibodies which precipitate at cooler temperatures, and not infrequently leads to renal failure/glomerulonephritis. The stereotypical histologic lesion of cryoglobulinemia is membranoproliferative glomerulonephritis, which takes the appearance on light microscopy of this heavily lobulated glomerulus.
Cryoglobulinemia is characterized by the presence of circulating antibodies which precipitate at cooler temperatures, and not infrequently leads to renal failure/glomerulonephritis. The stereotypical histologic lesion of cryoglobulinemia is membranoproliferative glomerulonephritis, which takes the appearance on light microscopy of this heavily lobulated glomerulus.
While cryoglobulinemia and MPGN display this link, it is important to realize that each term has its own classification scheme–this can be confusing since both cryoglobulinemia and MPGN each have 3 “Types”.
Cryoglobulinemia is classified based on the type of immunoglobulin present in the cryocrit:
Type I cryoglobulinemia is comprised simply of monoclonal immunoglobulins, typically IgM but less frequently IgG, IgA, or serum light chains. Not surprisingly, individuals with Type I cryos typically have a paraproteinemia (e.g., myeloma, Waldenstrom’s macroglobulinemia).
Type II cryoglobulinemia is when a monoclonal IgM recognizes and binds to polyclonal IgG’s, explaining why Type II cryos are IgM-IgG complexes.
Type III cryoglobulinemia is when a polyclonal Ig recognizes polyclonal Ig. Together, Type II & III cryoglobulinemia are referred to as “Mixed Cryoglobulinemia”, and these are the types most commonly associated with hepatitis C.
The MPGN Classification system is as follows:
Type I MPGN is a pattern which can be associated with many different diseases, of which cryoglobulinemia is one. Histologic findings include “tram tracking”/double contours of the GBM, hypercellularity of the glomerular tuft, and a lobulated appearance of the glomerulus. EM may show mesangial and subendothelial immune complex deposits.
Type II MPGN is also known as “dense deposit disease“, usually caused by the presence of C3 nephritic factor, and on EM shows ribbon-like electron-dense deposits within the glomerular and tubular basement membranes.
Type III MPGN, which is very rare, apparently includes a many of the features of Type I MPGN along with subepithelial deposits.


